Frozen Embryo Transfer (FET)
- Consultations
- Initial Consultation
- Fertility Assessment
- Fertility Treatments
- In-Vitro Fertislisation (IVF) & Intra – Cytoplasmic Sperm Injection (ICSI)
- Frozen Embryo Transfer (FET)
- Intra Uterine Insemination (IUI)
- Surgical Sperm Retrieval
- Egg Freezing
- Sperm Freezing
- Endometrial Scratch
- Embryo Glue
- EmbryoGen
This treatment is suitable for women with or without regular cycles and for patients with endometriosis. It involves taking oestradiol tablets to build up the lining of the uterus, followed by vaginal progesterone gel to make sure the lining is receptive to the embryo(s).
What will happen in my treatment cycle?
Consents
Before your cycle begins you will need to consent to the number of embryos to thaw and transfer. If you are having treatment with a partner, he/she needs to consent as well. The number of embryos to thaw and transfer will depend on your age, your medical history, the number of frozen embryos and whether they will be further cultured before transfer. Our staff will help you complete your consent form.
Down regulation
On day 1 of your cycle, phone the clinic. On day 21 of your cycle you will begin taking Buserelin as subcutaneous injections, once per day. This is a GnRH agonist that will stop your own production of FSH and LH, reducing the risk of spontaneous ovulation.
Down-regulation scan
After two weeks of Buserelin you will attend the clinic for a down-regulation scan. The scan will assess the endometrium lining of your uterus and see how active your ovaries are. If everything looks fine, you will be able to start your cycle. After you have your scan you will start to take hormone tablets (oestradiol) to build up your endometrium. Continue to take Buserelin as well.
Follicle tracking scans
After 11-13 days, you will have an ultrasound scan. We will measure the endometrial thickness and the size of any growing follicle. If the endometrium is more than 8 mm and no follicle is visible you are ready for your embryo transfer. If a dominant follicle larger than 14 mm is visible, you will have a blood test to see whether you have ovulated. If you have ovulated, your cycle will be cancelled because of reduced chances of success. If the endometrium is too thin, you will continue taking oestradiol and return after 7 days for a scan. If the endometrium does not thicken your cycle may be cancelled.
Additional hormones
When you are ready for your frozen embryo transfer, will start stop taking Buserelin and will begin to use progesterone (while continuing the oestradiol). This is to help make the endometrium receptive to the embryo(s). The start of progesterone equals luteal day 0.
Thaw and transfer
The embryos are thawed according to your consent. The majority of the embryos tolerate freezing and thawing well, but some may not. We normally do not call you, but decisions to thaw more might be needed and we therefore ask that you are available on the day of thawing.
The transfer procedure is quick and simple and usually completely painless. The embryos are gently transferred into the uterus by using a fine plastic tube (catheter).
Refreezing of embryos
Sometimes there may be more high quality embryos left after the transfer. Those embryos may be re-frozen with your consent. Please note that refreezing of surplus embryos comes with additional costs.
Hormone support
After the embryo transfer you will continue to take progesterone and oestradiol until the day of the pregnancy test. The lining of the uterus (endometrium) is normally supported with progesterone to help the embryo implant in the uterus. This is called "luteal phase support".
Pregnancy test
14 days after your luteal day 0 (the day you started taking progesterone) you will come to the clinic for a blood sample. This will measure the hCG level to determine whether you are pregnant or not.
What happens if the pregnancy test is positive?
Pregnancy scans
You will be asked to attend for a vaginal scan about three weeks after your pregnancy test (this is equivalent to seven weeks of pregnancy).
This scan is important to ensure that the pregnancy is in the correct place, that it is developing normally and to confirm how many pregnancy sacs there are. At this stage, the pregnancy should be clearly visible inside the uterus as a small sac with a tiny fetus within. It should be possible to identify a heartbeat at this stage.
If all is progressing normally, you will be discharged to your GP to arrange antenatal care. If problems are identified during these scans we will discuss the findings with you and make appropriate plans.
You should continue taking folic acid until 12 weeks of pregnancy.
Pregnancy outcome
We are required by law to notify the HFEA of the outcome of all treatment cycles. Please report the outcome of the pregnancy back to us. More information regarding this will be given to you when a pregnancy is confirmed.
What happens if the pregnancy test is negative?
A negative result means that pregnancy has not occurred this time. We realise that you may be very disappointed and the staff of the clinic are always available to offer support and advice. The counsellor is also available should you wish to have an appointment.
Appendix One: AC-FET with down regulation flowchart
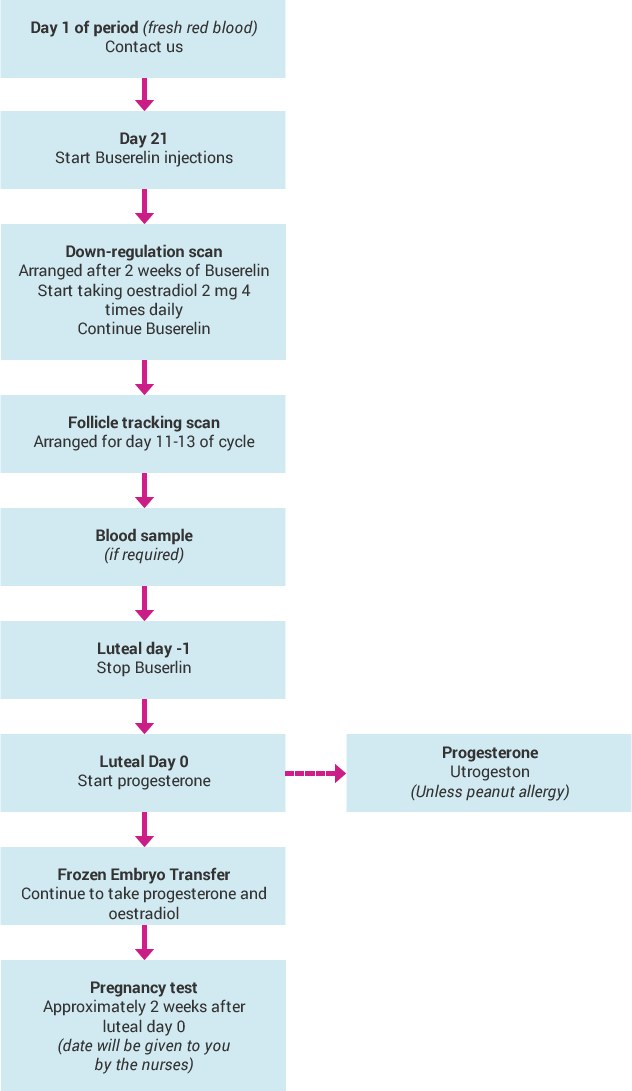
TESTIMONIALS
Mr Brook and the team were friendly, direct and very efficient. Overall an excellent service.


